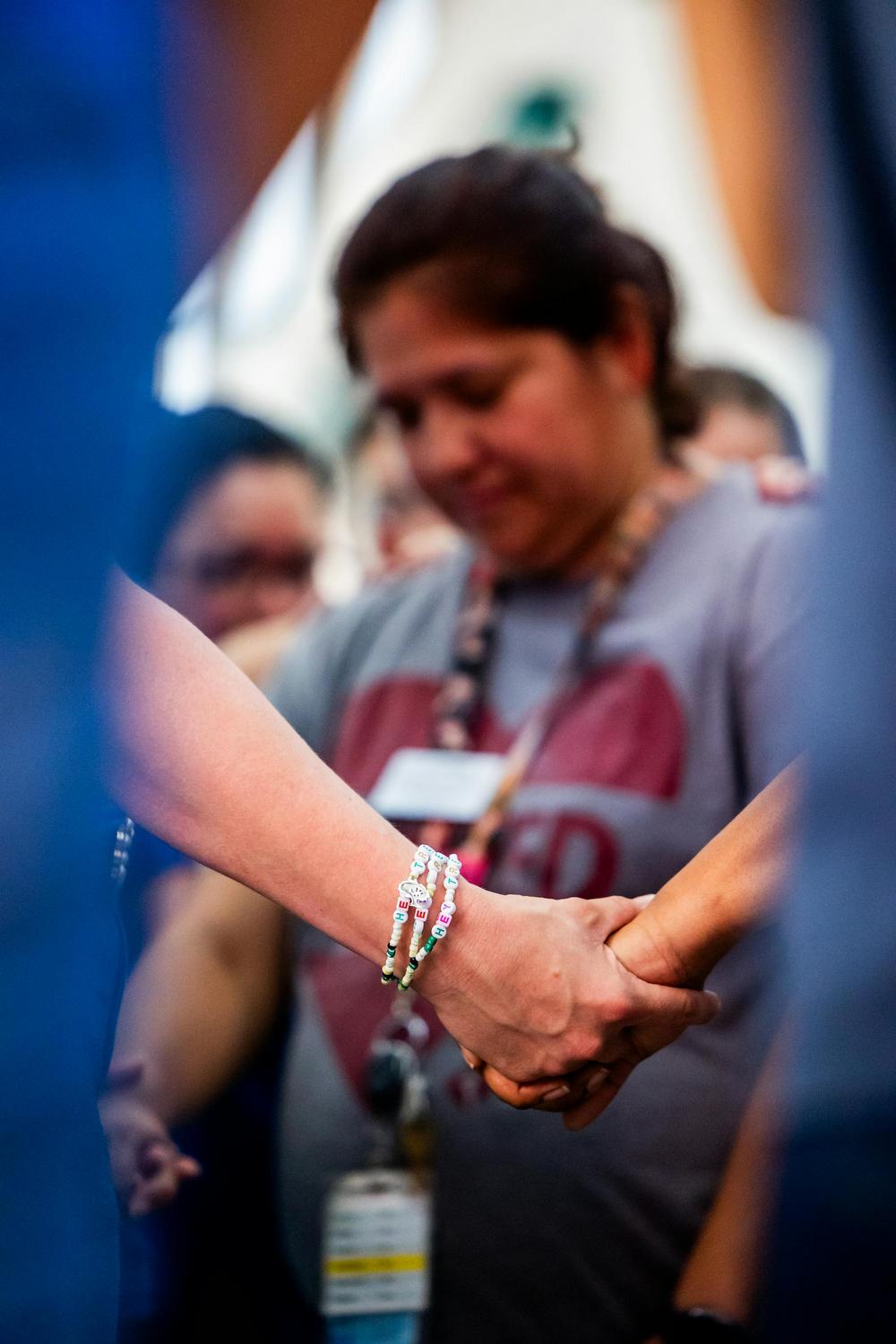The packed morning commute. Your colleague’s visible tension as they prepare for a difficult meeting. A parent’s anxious facial expression. These everyday encounters may be affecting your physiology in ways far more profound than previously understood. Recent neuroscience reveals that stress doesn’t merely stay with the person experiencing it—it transmits across individuals through measurable biological pathways, creating cascading effects that ripple through families, workplaces, and communities.
In 2026, as Australia grapples with unprecedented mental health challenges—with 38.8% of young people aged 16-24 experiencing mental disorders—understanding how stress moves between people has never been more critical. This phenomenon, known as stress contagion or social transmission of stress, represents not simply an emotional exchange but a documented neurophysiological process involving hormonal synchronisation, neural mirroring, and even chemical signalling.
What Is Stress Contagion and How Does It Differ from Regular Stress?
Stress contagion represents the transmission of stress responses from one individual to another, creating physiological and psychological changes in observers who have never directly encountered the original stressor. This distinguishes it fundamentally from standard stress reactions, where an individual responds to their own environmental challenges.
Research demonstrates that between 15-25% of an average person’s emotional state comprises emotions absorbed from others, according to collaborative studies from Harvard University and the University of California, San Diego. More remarkably, controlled laboratory observations reveal that 26% of individuals watching stressed persons through one-way mirrors experience significant cortisol elevation despite experiencing no personal stressor themselves.
The distinction proves crucial: stress contagion involves catching another person’s stress response through unconscious absorption of social and biological cues. An individual can develop measurable physiological stress markers—elevated cortisol, increased heart rate, heightened blood pressure—purely through proximity to someone experiencing stress, without any direct exposure to threatening stimuli.
This phenomenon operates through multiple transmission pathways simultaneously: neurological networks involving mirror neurons, hormonal cascades through the hypothalamic-pituitary-adrenal (HPA) axis, chemical signals detectable in human sweat, and behavioural modelling through observation. Each pathway contributes to the rapid spread of stress states across social networks, creating what researchers describe as “secondhand stress” with genuine physiological consequences.
How Does Stress Actually Transmit Between People?
The mechanisms underlying stress contagion reveal sophisticated biological systems designed for social connection that inadvertently facilitate stress transmission. Understanding these pathways illuminates why stress spreads so readily through close relationships and densely connected environments.
Mirror Neuron System Activation
The mirror neuron system represents a network of neurons that fire both when performing an action and when observing someone else performing that same action. Within milliseconds of encountering a stressed individual, these neurons automatically copy facial expressions, body language patterns, and vocal characteristics. This neural simulation creates corresponding emotional states in the observer without conscious intention or awareness.
Brain imaging studies identify several regions critically involved in this process: the insula translates observations of others’ experiences into similar visceral states within the observer; the anterior cingulate cortex activates during empathy and anxiety-related processing; the amygdala processes emotional salience and threat detection. These regions work in concert to create what neuroscientists term “neural synchrony”—the physical manifestation of one brain state influencing another.
Research demonstrates that individuals who display emotions more expressively on their faces serve as the most “infectious” transmitters. Physical proximity enhances neural contagion strength substantially, with romantic partners showing significantly stronger synchronisation patterns than strangers. Remarkably, even video observation maintains transmission capacity, though at slightly reduced rates (24%) compared to in-person observation through one-way mirrors (30%).
Hormonal and Physiological Synchronisation
The HPA axis—the body’s primary stress response system—activates in observers watching stressed individuals, creating a cascade of measurable hormonal changes. The hypothalamus releases corticotropin-releasing hormone (CRH), triggering the pituitary gland to release adrenocorticotropic hormone (ACTH), which signals the adrenal glands to release cortisol. Remarkably, cortisol levels in observers become proportional to cortisol levels in the stressed individuals they observe.
Within minutes of exposure to a stressed partner, observers experience cardiac activity changes matching the stressed person’s patterns. Heart rate increases, blood pressure elevates, and sympathetic nervous system activation markers become detectable. Research confirms that these changes occur automatically, without conscious awareness or voluntary control.
The transmission extends beyond cortisol to include adrenaline and alpha-amylase, marking comprehensive autonomic nervous system involvement. Interestingly, research shows no differences in aldosterone levels, suggesting the renin-angiotensin-aldosterone system (RAAS) remains insensitive to stress contagion, distinguishing which physiological systems participate in social transmission versus those that respond only to direct stressors.
Chemical Signal Pathways
Perhaps most surprising, stress transmits through chemical signals detectable in human sweat. Stressed individuals release “alarm pheromones”—stress-related chemical compounds including cortisol and adrenaline metabolites—that trigger fear responses in others through olfactory channels. This represents a primal evolutionary mechanism for rapid threat communication within groups, operating entirely outside conscious awareness.
Research exposing participants to sweat collected from highly stressed individuals demonstrates induced fearful facial expressions and heightened vigilance in receivers who never saw or interacted with the stressed person. This transmission mechanism functions effectively in enclosed spaces—offices, homes, vehicles—where stress pheromones accumulate in poorly ventilated environments.
The olfactory pathway enables stress transmission even without visual or auditory cues, explaining why individuals sometimes report feeling anxious or uneasy in certain spaces without identifiable triggers. The chemical dimension of stress contagion underscores its biological depth, operating through ancient sensory systems shared across mammalian species.
Who Is Most Vulnerable to Catching Stress from Others?
Susceptibility to stress contagion varies substantially across individuals, relationships, and contexts. Understanding these vulnerability factors helps identify populations requiring targeted support and protective interventions.
Relationship Closeness and Social Bonds
Research consistently demonstrates that relationship closeness represents the strongest predictor of stress transmission intensity. Romantic partners show the highest contagion rates, with 40% experiencing measurable stress responses when observing their partner under stress. Family members experience elevated transmission rates compared to friends, who in turn show stronger effects than acquaintances. Remarkably, even strangers demonstrate 10% rates of measurable cortisol increases when observing stressed individuals they’ve never met.
This gradient reflects how social bonds create enhanced receptivity to others’ emotional states. Stronger emotional investment translates to more active monitoring of partners’ wellbeing, increasing exposure to stress cues. Close relationships involve greater neural synchronisation during interactions, facilitating faster and more complete transmission of physiological states between partners.
Empathy and Personality Characteristics
Individuals with higher empathy levels demonstrate faster psychophysiological reactivity to others’ stress, with decreased latency between observing stress and experiencing physiological responses. This enhanced sensitivity creates both a strength—the capacity for deep emotional connection—and a vulnerability to absorbing others’ distress.
Specific personality traits modulate susceptibility significantly. High neuroticism increases vulnerability to stress contagion, as does low conscientiousness. Conversely, an internal locus of control—belief in personal agency over outcomes—acts as a protective buffer, whilst external locus of control increases transmission susceptibility. Trait anxiety predisposes individuals to catching others’ stress more readily, creating potential feedback loops where anxious individuals both transmit and receive stress more efficiently.
Demographic and Population Factors
Australian mental health data from 2020-2022 reveals concerning patterns in stress vulnerability. Young people aged 16-24 show the highest prevalence of mental disorders (38.8%), with young women particularly affected (45.5% compared to 32.4% in young men). This demographic experiences elevated susceptibility to stress contagion through multiple pathways: greater social media exposure amplifying emotional contagion, developmental sensitivity during identity formation, and higher baseline anxiety creating receptivity to environmental stress cues.
Marginalised populations demonstrate compounded vulnerability. Australian research shows LGBTIQA+ youth experience 77% rates of high psychological distress, whilst First Nations young people face 59% rates. Unemployment correlates with 36.1% mental disorder prevalence versus 22.8% in employed individuals. These disparities suggest that chronic stress exposure, social marginalisation, and limited access to protective resources create enhanced susceptibility to additional stress through social transmission.
What Are the Health Consequences of Repeated Stress Contagion?
Chronic exposure to others’ stress creates documented health impacts extending far beyond temporary discomfort. The accumulated burden of repeated stress contagion manifests in measurable physiological, psychological, and behavioural changes with long-term health implications.
HPA Axis Dysregulation and Chronic Effects
Repeated stress contagion exposure triggers sustained HPA axis activation, eventually dysregulating this critical stress response system. Chronically elevated baseline cortisol develops, accompanied by flattened diurnal cortisol rhythms—the normal rise and fall across the day becomes blunted. In some cases, chronic exposure leads paradoxically to hypocortisolism, where the exhausted system produces insufficient cortisol, similar to patterns observed in post-traumatic stress disorder.
These hormonal disruptions cascade into multiple health systems. Increased inflammation markers appear, alongside elevated cardiovascular disease risk. Immune system suppression increases vulnerability to infections and delayed wound healing. Sleep architecture deteriorates, with difficulty initiating and maintaining restorative sleep cycles. Metabolic dysfunction emerges, including increased risk of weight gain and metabolic syndrome. The neurotoxic effects of chronic cortisol elevation contribute to cognitive decline and mood disorder development.
Healthcare workers and family caregivers demonstrate particularly pronounced effects, termed “caregiver stress syndrome.” These individuals show measurable health decline across multiple parameters, including cardiovascular function, immune competence, and mental health status. Family members of trauma survivors can develop secondhand post-traumatic stress disorder, experiencing intrusive thoughts, hypervigilance, and avoidance behaviours despite no direct trauma exposure.
Cognitive and Workplace Impacts
Stress contagion profoundly affects cognitive functioning and workplace dynamics. Stressed brains default to rigid, habitual thinking patterns, reducing cognitive flexibility and creative problem-solving capacity. Decision-making quality deteriorates, with increased reliance on heuristics rather than careful analysis. Perspective-taking ability diminishes, undermining collaboration and conflict resolution.
Australian workplace data reveals concerning patterns: over 80% of workers globally report experiencing work stress, with over 25% identifying employment as their primary stressor. Personal finances represent the leading cause of stress for 49% of Australians, followed closely by work and family relationships. In open-plan office environments, which have proliferated despite evidence of stress amplification, visible stress behaviours—rushing, appearing overwhelmed, skipping meals—create team-wide stress activation.
Leadership stress proves particularly contagious, flowing downward through organisational hierarchies more readily than upward. When managers display visible stress, entire teams experience elevated cortisol, reduced productivity, and increased conflict. Innovation suffers as stressed brains struggle to generate breakthrough ideas, defaulting instead to familiar solutions. Team cohesion fragments as individuals withdraw socially to protect against additional stress exposure.
Intergenerational Transmission Patterns
Perhaps most concerning, stress contagion creates intergenerational effects with lifelong implications. Infants and children show elevated baseline cortisol when mothers experience chronic stress, with blunted cortisol response patterns similar to those observed in adult trauma populations. Children of anxious parents demonstrate 2-3 times increased likelihood of developing anxiety disorders themselves, with 33% developing diagnosable psychiatric conditions.
These effects persist even when controlling for genetic factors, demonstrating that environmental transmission through stress contagion represents a primary mechanism. Same-sex parent transmission shows stronger effects than opposite-sex transmission, suggesting modelling and vicarious learning pathways dominate over genetic inheritance. The specific anxiety symptoms—social phobia, generalised anxiety, panic—show disorder-specific parent-child matching, further supporting learned rather than inherited transmission.
Early stress exposure creates sensitised stress response systems with lower activation thresholds throughout life. These individuals demonstrate increased vulnerability to anxiety and mood disorders, altered emotional regulation capacities, and potential epigenetic changes—modifications in gene expression without DNA sequence changes—that may themselves transmit across generations. Research on Holocaust survivors’ offspring demonstrates altered HPA axis function decades after parental trauma exposure, illustrating the profound and lasting impact of stress transmission across generations.
How Can We Protect Ourselves and Others from Stress Contagion?
Understanding transmission mechanisms enables development of effective protective strategies operating at individual, relational, and organisational levels. Evidence-based approaches offer genuine capacity to interrupt stress contagion cascades and promote resilience.
Individual Protective Practices
Conscious emotion regulation skills provide first-line defence against stress contagion. Cognitive reappraisal—deliberately reframing situations as manageable rather than threatening—changes physiological responses measurably. Mindfulness practices enhance awareness of absorbed emotions, creating choice points for responding rather than automatically mirroring others’ states. Developing emotional granularity—the ability to distinguish specific emotions precisely—enables more nuanced responses to stress exposure.
Interestingly, research demonstrates that conscious facial muscle control can interrupt mirror neuron activation. By deliberately relaxing facial muscles when encountering stressed individuals, observers reduce their own stress response activation. This seemingly simple intervention disrupts the automatic mimicry that initiates stress contagion, though it requires awareness and practice to implement effectively.
Physical practices offer robust protection. Regular exercise demonstrates stress-buffering effects through multiple mechanisms, including improved HPA axis regulation and enhanced parasympathetic nervous system activity. Nature exposure reduces stress markers reliably, with even brief periods outdoors showing measurable benefits. Breathing exercises activate the vagus nerve, promoting parasympathetic “rest and digest” responses that counteract sympathetic stress activation.
Relational and Social Buffering
Social buffering represents a powerful counterforce to stress contagion, operating through the same neural and hormonal systems that transmit stress. The presence of calm, supportive individuals reduces stress response magnitude by approximately 50% in research studies. This protection requires adequate availability of non-stressed individuals within social networks—a concerning challenge given current prevalence rates of mental disorders affecting 21.5% of Australians aged 16-85.
Active listening and empathic validation create co-regulation—synchronised calming between individuals that restores physiological balance. Physical touch, particularly hand-holding with trusted partners, activates oxytocin systems that promote feelings of safety and reduce threat response activation. Secure attachment relationships provide robust protection across the lifespan, buffering against both direct stressors and socially transmitted stress.
Research on parent-based interventions demonstrates that treating one family member’s anxiety protects others from developing or maintaining anxiety symptoms. Two-year follow-up studies show stable positive outcomes, confirming that addressing stress in key individuals creates ripple effects benefiting entire family systems. This finding has profound implications for healthcare approaches: targeting parents, leaders, and primary caregivers offers multiplied returns through reduced stress transmission to dependent individuals.
Organisational and Environmental Strategies
Workplace and organisational interventions address structural factors amplifying stress contagion. Clear communication reduces uncertainty-based stress that spreads rapidly through teams. Strong team psychological safety—environments where individuals feel secure expressing concerns without fear of negative consequences—buffers stress transmission by enabling early intervention before stress escalates.
Leadership training focused on emotional regulation and supportive presence creates powerful protective effects cascading through organisations. When leaders model calm responses to challenges and validate team members’ experiences, they interrupt stress contagion chains whilst simultaneously building team resilience. Flexible work arrangements allowing control over work conditions and adequate recovery time prevent chronic stress accumulation that increases contagion susceptibility.
Environmental design considerations prove surprisingly important. Private spaces for focused work or emotional recovery reduce constant exposure to others’ stress cues. Natural light, plants, and nature views provide passive stress reduction. Air quality improvements may reduce stress pheromone concentration in enclosed spaces, though research on this mechanism remains limited.
Mental health resource accessibility represents foundational protection. Yet Australian data reveals significant gaps: only 45.1% of individuals with mental disorders accessed health professional support in the past year, despite 17.4% of the population aged 16-85 seeking mental health consultation. Wait times, costs, and stigma create barriers that leave individuals vulnerable to both direct stress and social transmission without adequate support.
Moving Forward: Implications for Wellbeing in Connected Societies
The neuroscience of stress contagion reveals that human interconnection creates both vulnerability and opportunity. Whilst stress transmits readily through families, workplaces, and communities via measurable neurological, hormonal, and chemical pathways, the same systems enable transmission of calm, support, and resilience. Understanding social transmission of stress transforms how we conceptualise mental health—not as purely individual phenomena but as deeply social processes requiring both personal and systemic interventions.
Australia’s mental health landscape in 2026 reflects concerning upward trends, particularly amongst young people, with 49% of youth experiencing high or very high psychological distress. Financial stress, employment precarity, housing insecurity, and digital connectivity demands create chronic stressor exposure that sensitises populations to stress contagion. These structural factors intersect with individual vulnerabilities, creating cascading effects that propagate through social networks.
Research demonstrates unequivocally that stress involves measurable physiological transmission between people who never directly encounter stressors themselves. This finding necessitates expanded approaches addressing not only individual stress management but also relational dynamics, organisational cultures, and community-level stress reduction. Treating stress in key individuals—parents, leaders, primary caregivers—creates protective ripple effects extending far beyond the treated individual.
The encouraging message within stress contagion research lies in its reversibility. Calm, regulated individuals buffer and protect others through the same neural and physiological systems that transmit stress. Conscious cultivation of regulated states, supportive relationships, and healthy environments creates positive contagion effects. In interconnected societies, individual wellness becomes a collective contribution, whilst collective wellness supports individual resilience—a reciprocal relationship offering genuine hope for addressing mental health challenges at scale.
Can stress contagion occur through digital interactions or only in person?
Stress contagion operates effectively through digital channels, though potentially at reduced intensity compared to in-person transmission. Research demonstrates emotional contagion occurring without face-to-face interaction—through social media exposure, video calls, and even text-based communication. While the absence of chemical signalling (such as pheromones) might attenuate the effect, the impact of nonverbal cues like facial expressions and tone still facilitates the transmission of stress digitally.
How quickly does stress contagion affect an observer’s physiology?
Stress contagion initiates remarkably rapidly through multiple pathways. Mirror neuron activation and autonomic nervous system responses begin within milliseconds of encountering stress cues, with heart rate changes detectable within minutes. The hormonal cascade through the HPA axis, however, may take 15-30 minutes to reach peak cortisol levels after exposure. Chronic exposure results in accumulated physiological changes over weeks to months.
Is everyone equally susceptible to catching stress from others?
Individual susceptibility to stress contagion varies based on factors such as relationship closeness, empathy, personality traits, and demographic characteristics. Romantic partners and close family members tend to exhibit higher transmission rates compared to strangers. Traits like high empathy and neuroticism increase vulnerability, while an internal locus of control can offer protection. Additionally, demographic groups such as young people and marginalised populations may show heightened susceptibility.
Can positive emotions spread as easily as stress and negative emotions?
Research indicates that negative emotions, including stress, tend to spread more readily than positive emotions—a phenomenon known as negativity bias. While positive emotional contagion is possible, it often requires more deliberate cultivation and supportive conditions to counterbalance the rapid transmission of negative states. Increasing the presence of calm and positive individuals in a social network can help mitigate the dominance of negative contagion.
How does treating one family member’s stress affect other family members?
Treating one family member’s stress can have protective ripple effects throughout the entire family system. For instance, effective intervention for a parent’s anxiety has been shown to reduce the risk of anxiety disorders in their children by interrupting the transmission pathways of stress. This interruption happens through reduced modeling of anxious behaviors, decreased exposure to stress signals, and improved family communication dynamics, ultimately benefiting all members.